In a New York sitcom, I’d never sit at the edge of my bed, head cupped in my hands, saying, “I’d like you to get tested for STIs,” and hesitantly add, “Did you do this on purpose?” Kids, Ted actually met your mother because his condom broke during a one-night stand. On a tangential note, in a Delhi sitcom, I’d probably give birth to triplets just as a seductress, who can probably make money off uploading eye makeup tutorials on YouTube, murders my husband.
On a sultry night in July, my date and I looked into each other’s eyes. “Ah,” he fumbled, “this has never happened before!” He gestured frantically towards the torn condom he was still wearing. “What do we do now?” It wasn’t a question as much as commiseration. Obviously, I would take the emergency pill and still spend the week preceding my period stomping around my house, bugging my very patient flatmates, “What if there’s a bun in my oven?” With the situation at hand, a part of my brain wondered if he’d tampered with the condom, and another rummaged through the memory of an absurdly painful menstrual cycle when I previously took the emergency pill. As scared as I was, I was more grateful – it is a privilege to be able to walk to the nearest (or even farthest for that matter) pharmacy and ask the man at the counter for the 72-hour pill without being murdered to preserve family honour; nausea, bloating, dizziness, and bleeding are minor inconveniences in comparison. Despite being available over the counter, emergency contraception is not widely advertised or stocked because of government policies. These policies were further tweaked in 2019 to mandate a doctor’s prescription for the sale of birth control pills such as Saheli and Apsara, a step counter-intuitive to accessibility as well as de-stigmatisation of women-dealt birth control. It doesn’t reassure one either that these pills are usually named in a manner that fuses agency with alarm – Unwanted 72, iPill, Take Action (steering clear of which Pregnon evokes the figure of a bearded French musician nibbling on a baguette).
But sometimes Plan B isn’t too bad. Especially when you’re spared Plan C – an unnecessarily bloody and painful abortion; unnecessarily bloody and painful because if scientists focussed on making it less so, we’d have got there, but they’d rather use money and resources to make an A.I.-backed blowjob gadget! Well, anyway, as a sexually active woman who doesn’t want to get pregnant, I can still pop birth control pills, shove a hormone-secreting plastic ring up my vagina, cover my cervix with an unfashionable silicone cap, insert a copper-releasing device into my uterus, irreversibly tie my fallopian tubes, and so on and so forth, so what am I complaining about? Unsurprisingly, the Pill’s conception is yoked to women’s emancipation – it is after all a discreet tablet handing you control over your body. Its hormonal constitution when it was introduced in the market exceeded by over five hundred percent what is manufactured today. At the time, the Pill allowed women to finally dissociate sex from procreation, enter the workforce and gain economic independence, and explore personhood outside their primary responsibility of home-making as well as exponentially increased their susceptibility to severe medical conditions, including heart attack and stroke. Win some, lose some.
We are told we pay a fair price for the freedom contraception affords us. Don’t want to have kid after kid because you care about your career but don’t know how to bring it up with your Anti-Choice cis male partner? Don’t worry. Most birth control methods you can avail of will not impact him in the least! Some nights I worry that if birth control for men is indeed released, clinical trials of which were suspended in 2016 as its side effects, incidentally the same as what women have been dealing with for ages, were just not worth it, it would be named Fuckboi. At present, two birth control methods exist for men – condoms and vasectomy. However, because conception occurs in a woman’s body, it is assumed to be her responsibility to prevent it when it is unwanted.
Science and technology aren’t outside the purview of hetero-patriarchy. As we grapple with a pandemic at a global scale, biases in medicine and healthcare have further come to the surface, particularly when we consider whose wellbeing is privileged and over that of whom, manifest in instances ranging from the US monopolising COVID-drug Remdesivir to the direness of how the response to COVID threatens women’s and girls’ sexual and reproductive health and rights (SRHR) as well as the health and economic security of LGBT people, and revealing and making more profound inequalities of gender, class and caste, race and even that between the First and the Third World. As we think more than ever before about safety, we have an opportunity to look at it, in context of contraception, beyond preventing unwanted pregnancy and as affirming bodily agency and integrity.
A sundry collection of birth control methods are available (some more readily than others) but isn’t it odd that only condoms also protect against STIs? In fact, apart from being pretty ineffective at what it’s supposed to do, spermicide may actually increase the risk of contracting such infections! The suffix -cide means ‘killer of’. Apart from being used in dull Geography lessons where we drew tables to compare manure and pesticide, -cide finds itself a part of rather ominous words such as genocide and infanticide. Spermicide certainly could have been named better, not only because it doesn’t quite match up to the ‘-cide’ but also because it signifies violence, the intention to attack and kill rather than to prevent. As mentioned earlier, science is by and for our world and is thus, not immune (even though it is held in high regard as an ‘objective’ and ‘hard’ institution) to its politics. Many a time, the militaristic attitudes of States are reflected in the language we use to describe what/who we perceive as an outsider. I doubt Paracetamol would sell at all if it says, “Sit down and have a cup of tea with your flu before bidding it goodbye!” but how might innovation alter if the discourse of medicine focused on healing instead of kitanu ka khaatma (the extermination of germs)?
Still, from intracytoplasmic sperm injection (ICSI) and abortion pills to HPV vaccines and PReP drugs, science has transformed the way we engage with the world and one another. My parents often dramatise the arduousness of earlier times. “When I was young, I had to eat everything that was put on my plate!” with an implied, “Look at you, such a picky eater!”, or even “When I was pregnant with you, I had to wait two hours just to get through to Papa (who was at work in another state at the time) on call. Imagine if I’d suddenly gone into labour!” Quite unlike the world they grew up in and knew, my world grew bigger and bigger with me. With the Internet, we could watch the sun set in a previously remote and unheard-of town, eavesdrop on conversations between whales, find validation for who we were, especially if we didn’t quite fit in in ‘real’ life, and build community with anyone anywhere in a click, regardless of time and distance. Despite all this, science has not expanded our contraceptive choices enough. A cursory Google search for upcoming innovations in contraception yields woefully disappointing results that I am convinced only cis male authors can call ‘exciting’ in headlines. A hormone-releasing implanted microchip, intrauterine devices that may be “better tolerated” and creams may prevent pregnancy but don’t help in building a sustainable and sexuality affirming environment for people of all sexual and gender identities and sexualities. Options like the male birth control pill, reversible inhibition of sperm under guidance (RISUG) or a gel that doesn’t completely mess up one’s hormones neither receive adequate funding or attention nor appear urgent in technological imagination. As we try to understand and recalibrate our patriarchally organised world, we need to find better and safer ways in which we can delight in sexual expression without fearing the possible unwanted consequences: a pregnancy or STIs.
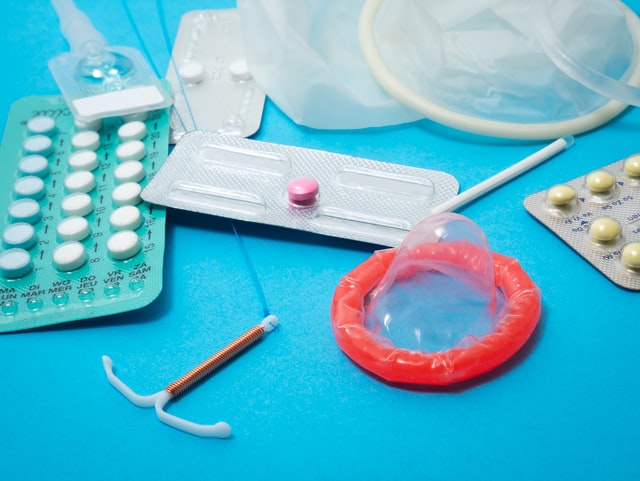
Cover Image: Unsplash